A macular hole is a full-thickness tissue defect that produces a gray or black spot in the macula. The macula is a small area in the center of the retina that is responsible for straight-ahead or focused vision. The very center of the macula is also the thinnest part of the retina, making it susceptible to holes, particularly as a person ages.
Although a macular hole may gradually enlarge, peripheral vision remains, and straight-ahead vision is almost never completely lost. Most macular holes develop as a result of the vitreous gel pulling on the delicate macular tissue. Unlike tears in the peripheral retina, a macular hole does not typically lead to retinal detachment.
Once a macular hole forms in one eye, the risk of one developing in the other eye may be as high as 10 or 15 percent. An examination and periodic monitoring are recommended.
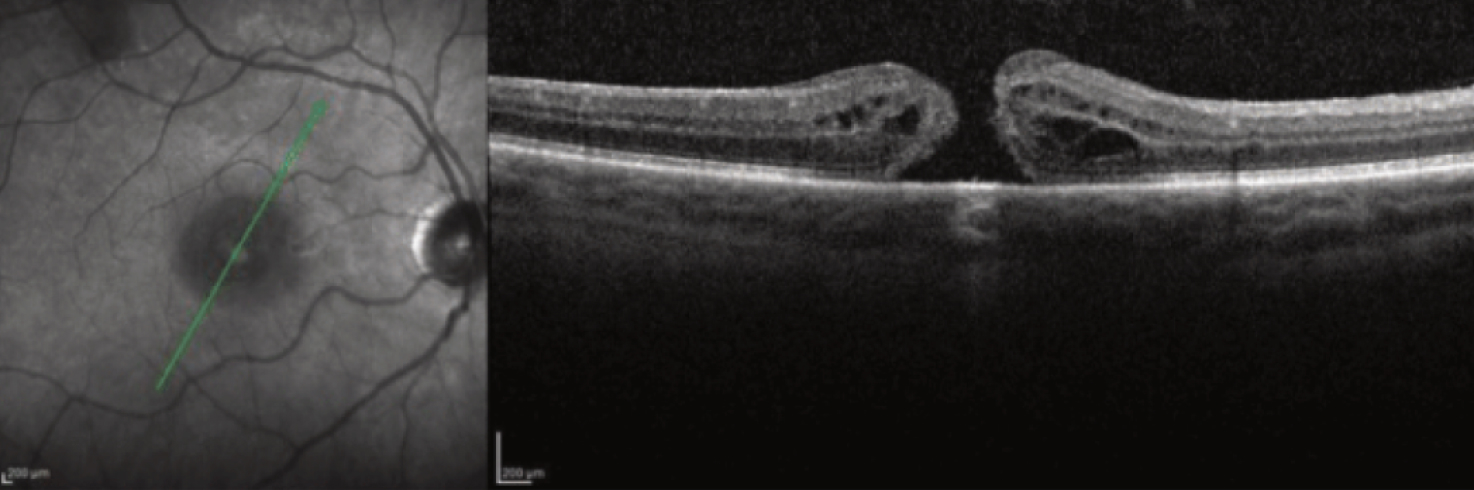
Usually, macular holes can cause:
The severity of macular hole symptoms is dependent on the individual and the extent of the condition. These symptoms can also be caused by other retinal disorders. In any case, it is recommended to seek treatment from a retinal specialist at the first sign of symptoms.
The vitreous gel separating from the retina with age is the most common cause, and is more common in those aged 55 years and older.
Other potential macular hole causes include:
The condition is also more common for women than men.
A complete and comprehensive eye examination is important to diagnose and assess the hole, including vision testing, eye drops to dilate the pupils, and a complete examination of the front and back of the eye. A driver should accompany the patient during the eye exam, as pupillary dilation may create near-vision blurring
People with a macular hole may require several types of tests to evaluate their condition, including:
Vitrectomy surgery is the usual macular hole treatment. A vitrectomy is an outpatient surgery usually performed under local anesthesia to remove the vitreous gel that caused the hole.
In order to seal the hole closed, your doctor will replace the gel with a temporary gas bubble at the time of surgery. This bubble will severely limit the vision in the operated eye for a few weeks, depending upon the type of gas bubble used. The body eventually absorbs this gas bubble and replaces it with natural eye fluids.
After macular eye surgery, most people attain some degree of noticeable visual improvement, but the improvement is usually gradual (weeks to months). It is relatively common to have cataract development or progression months after surgery. Your surgeon will review procedure risks, benefits, and alternatives with you and make tailored recommendations based on your specific case.
If you have any signs or symptoms of macular hole, contact us today to meet with a Mid Atlantic Retina specialist. Our team can work with you to protect your vision and minimize your complications.
Are you curious about macular hole stages? What about the recovery time from macular hole...