- On this page: Symptoms
- Causes and Associations
- Testing
- Treatment
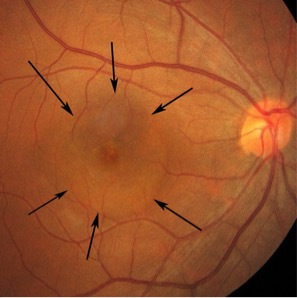 Central serous chorioretinopathy (CSCR), also known as central serous retinopathy, is a condition that causes fluid to build up underneath the macula, the center of the retina. Fluid leaks from a layer of blood vessels that run beneath the retina called the choroid.
Central serous chorioretinopathy (CSCR), also known as central serous retinopathy, is a condition that causes fluid to build up underneath the macula, the center of the retina. Fluid leaks from a layer of blood vessels that run beneath the retina called the choroid.
CSCR is often a chronic disease. It may recur in 20 to 30 percent of patients, and some degree of permanent visual loss is more likely in recurrent or prolonged cases.
Central serous chorioretinopathy symptoms can include:
The exact cause of CSCR remains unknown, but associations can include:
Central serous chorioretinopathy is more common in men, primarily between the ages of 25 to 50 years. Those with a history of CSCR should avoid steroid medications if possible.
A comprehensive eye examination is important to assess CSCR, including vision testing, eye drops to dilate the pupils, and a complete examination of the front and back of the eye. It is best if a driver accompanies the patient during their eye exam, as pupillary dilation may create near-vision blurring.
People with CSCR may undergo several tests to evaluate their condition, including:
In most cases, the fluid under the retina resolves spontaneously over several months. Patients are usually followed without treatment, but treatment may be recommended for those who maintain subretinal fluid after a few months. The final visual outcome is usually good, though not always perfect, due to permanent damage to the retinal tissue.
Treatment selection is based on the severity of the condition and the individual patient and may include the following:
Laser photocoagulation is performed in the office setting. A laser delivers a split-second burst of intense light energy to treat leaky retinal blood vessels or promote the shrinkage of abnormal blood vessels. If there is too much bleeding in the retina, laser photocoagulation cannot be performed.
Photodynamic therapy (PDT) is a two-step procedure that can be performed in the doctor’s office. A light-activated drug is injected into the patient’s arm and activated in the eye with a non-thermal laser. Treatment may need to be repeated over the course of one to two years in order to promote vision stabilization.
Intravitreal injections are used to treat many retinal conditions. With this treatment, anti-vascular endothelial growth factor (VEGF) inhibitors or steroids are injected directly into the eye. This procedure is performed in the office and requires only a local anesthetic. Intravitreal injections may be administered as frequently as once a month (depending on the condition being treated) in order to maintain eye health and optimize vision.
If you have any signs or symptoms of CSCR, contact us today to meet with a Mid Atlantic Retina specialist. Our team can work with you to protect your vision and minimize your complications.